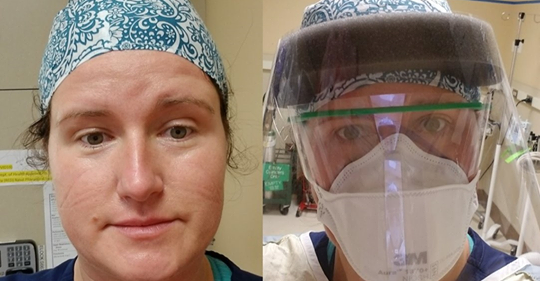
Frontline ICU Nurse in the COVID battle says, “My Purpose Is To Help My Patients Feel Better.”
Earlier in her career, Tiffany Wolfsberger worked as an emergency room nurse for two years. While she learned a lot in the fast-paced ER environment, it was tough to develop a connection with the patient. If the patient’s ailment was fixed, that person left the hospital. If it was mitigated yet further care was necessary, the patient was transferred to another section of the hospital. The ER was too transactional for Tiffany. She transferred to the intensive care unit, where for seventeen years, Tiffany Wolfsberger, has served as an ICU nurse at Regions Hospital in Maplewood, MN, and has worked to help very sick patients get better.
When asked about her purpose, she says, “To do anything I can do – physically, mentally, spiritually, emotionally – to help my patients feel better.”
In the past two weeks, the ICU at Regions has been under siege with COVID-19 cases. She’s seen more COVID patients enter her unit. Tiffany said, “Yesterday, we had 17 nurses on the floor, usually we have nine nurses.”.
By the time patients reach the ICU, they are very sick. Many have trouble breathing on their own, are on ventilators, a number are on dialysis, with their blood pressure increasing. With the influx of patients from nursing homes, many of whom have chronic health conditions, the spread of COVID-19 is extremely aggressive. Tiffany says, “It’s truly something we haven’t seen.”
What has been most difficult for Tiffany and her colleagues since the outbreak of the coronavirus in Minnesota in mid-March, has been the inability of family members to visit their loved ones. As Tiffany described, “The absence of family of the patients has been so hard. Before COVID, we often learned from the family things about their loved one. ‘What does an expression look like? Are they in pain? Do they like their feet tucked in?’ Just simple things.”
She continued, “They’re the patient’s real support. We’re there to help them but there’s an emptiness to not having that. The rooms and hallways at the hospital are empty. The parking garage is empty.”
“Now, when we talk with the family, there is only one contact person per family speaking with us. That’s so hard for the family members. It’s such a difficult time for them. The family is truly missed. In normal times, I do my best to get to know the family. They become comfortable with me as they get to know me. They know I’m there to help them.”
Tiffany added, “I want to be that person for them. I look forward to getting to work and seeing if someone is getting better. At home, I’ll wonder, ‘Is he getting better?’ When I get to work, I’ll check the ventilator settings. Have they been adjusted, to show he’s getting better? If they are not getting better, Tiffany works to provide even more support to the family.
On April 30, KARE 11’s Brandon Stahl and Lou Raguse ran a story “In her words: Dying from COVID, but not alone”, describing what it was like to be the only person able to care for 60-year old Don Lydick, who was dying from COVID. They interviewed Tiffany. Part of that story is retold below.
“I came into Don’s life just at the end. I had been off work and just had come back. Don was on our floor for almost two weeks, very sick and needed ventilator support early on. The virus just took over. It changed his organ function. It’s just such a vicious virus. To see what it is doing to patients; it’s like nothing I’ve ever experienced.
Don got to the point where he couldn’t tolerate going on his back. He was on his belly for almost, I want to say four to five days. That was the only way we could keep him alive. There was nothing more we could do for him.
I first called Joanne (his sister) and explained that his face might look a little swollen because he’s been on his stomach and she might not recognize him. She was very nervous to see him. I let her know that I could make it so that she would just see the back of him, so it would look like he’s just sleeping. And it would give her peace. She said that would be great.
She said, “Can you promise me that someone’s going to be there to hold his hand and pray with him?” And I said I can promise that.
The next step was to get the video iPad, and I did a test call in the conference room. I made sure to take off all of my goggles and face mask and everything, just so they could really see who was going to be with their brother in his final moments, that I really truly was going to be there for him and treat him like he was my brother.
And I let them talk to him. It was hard to not just have tears in your eyes, to look at this monitor with loved ones saying goodbye on a screen. Nothing prepares you for that moment. And that moment will never leave me.
They said their goodbyes, they encouraged him to go find his mom and his dad. Told some funny stories. We said a prayer together. I told them I would call Joanne when he was gone.
I went back in, we made him comfortable; turned off any medication that was artificially raising his blood pressure. And I held his hands and talked to him. I talked to him like he could hear me. I told him how his sisters told him that he was loved, and I tried to treat him as if he was my brother.
I sang “When I go down to the river to pray.” I actually noticed some tattoos and said you know I would love to hear the stories about these. I rubbed his head, his shoulder, to just let him know I was there with him.
You sit and you hold somebody’s hand and you look at their breathing and how it changes. And then you just see someone so tired at peace. You see the monitor, the heart slowing and slowing and those final breaths. What I saw was somebody’s son. He took his last breath, about two hours after. I stayed with him. I said a prayer with him.
Afterwords, I just took a moment to absorb what happened. I called Joanne, I told her about how Don looked, how peaceful it was. She was very grateful. She was surprised. “You were there the whole time?” I told her: “I promised you that he would not die alone. And I was in there until he did.”
Driving home, that’s when I really let my emotions go. Because you really have to keep it all together, you don’t want to make the patient sense your sadness. But that drive home was a hard one. I really knew there was going to be more Don’s in my future. It’s sad. It’s scary, and it just really, really affects you.
I know that we are no substitute for a family member, a wife, a sister. I know that. But I do want people to know that we’re struggling with this just as much as they are. And we are all working to make this not be the case – that no one will die alone. We all stand together. We just want them to know, that we’re going to be there for them.”
When Don Lydick, a former U.S. Navy nurse took his last breath on April 10, he was not alone. Tiffany Wolfsberger held his hand while he passed. As so many ICU nurses around the country are doing today with so many victims of COVID-19. They are our frontline heroes.
Married for fourteen years to husband John, a St. Paul firefighter, together they are raising their 12 year old son and 10 year old daughter. Tiffany is passionate about her family, her work and her patients.
As National Nurses Week concludes, it is important we recognize nurses like Tiffany whose purpose is “To do anything I can do – physically, mentally, spiritually, emotionally – to help my patients feel better”, for the loving care and support they give patients and their families during their hour of need. These healthcare professionals have an enormous impact on making the world a better place. Tiffany Wolfsberger is making an enormous impact. Thank you, Tiffany.












Trackbacks & Pingbacks
[…] John’s wife, Tiffany Wolfsberger, is an ICU nurse and her story was shared on May 12, 2020 https://theboltongroup.com/frontline-icu-nurse-in-the-covid-battle-says-my-purpose-is-to-help-my-pati… […]
Leave a Reply
Want to join the discussion?Feel free to contribute!